Development of New Tm-170 Radioactive Seeds for Brachytherapy
Amal Hwaree Ayoub, PhD Candidate
Department of Biomedical Engineering, Ben-Gurion University of the Negev,
P.O. Box 653, Beer Sheva, Israel
Corresponding Author: Phone: +972-8-647-9604, Fax: +972-8-647-9632,
E-mail: hwaree@bgu.ac.il
Jacob Gopas, Ph.D.
Department of Microbiology and Immunology, Faculty of Health Sciences,
Ben-Gurion University of the Negev and Department of Oncology, Soroka University Medical Center
P.O. Box 653, Beer Sheva, Israel
Gad Shani, PhD
Department of Biomedical Engineering, Ben-Gurion University of the Negev,
P.O. Box 653, Beer Sheva, Israel
Running title: Tm-170
Brachytherapy source
Ayoub, A. Gopas, J. and Shani, G. Development of New Tm-170 Radioactive Seeds for Brachytherapy
ABSTRACT
Purpose: To investigate the use of Tm-170 seeds for brachytherapy in comparison to Iodine-125 seeds.
Methods and materials: In vivo experiments were done in Balb/C mice. The KHJJ murine mammary carcinoma was selected as the tumor model because it is radio-resistant. KHJJ tumors were implanted on mice thighs and tumor growth was recorded as a function of time. When tumors reached the diameter of 7.5�9 mm, four groups of 20 tumor-bearing mice each, were implanted in the tumor as follows: 1. With Tm-170 seeds of activity 2.54 mCi, 2. With I-125 seeds of 0.5 mCi nominal activity (equal gamma dose to that of the Tm-170 seeds), 3. With control dummy seeds (empty titanium tubes of dimensions similar to Tm-170 seeds, that went through the same activation process as the real seeds) and 4. Control untreated mice.
Results: The results show that control tumors and tumors implanted with the dummy seeds grew exponentially with time. Implantation of I-125 seeds resulted in the disappearance of 25% of the tumors (cured mice), 25% of the tumors grew slower than the control tumors (growth delay), and 50% of the tumors were not affected by the radiation. Implantation of Tm-170 seeds resulted in 60% cure, 20% growth delay and 20% of the tumors were not affected by the radiation.
Conclusions: Tumors implanted with Tm-170 seeds were exposed to a smaller photon dose than those implanted with I-125 seeds; nevertheless Tm-170 seeds yielded significantly better results. Brachytherapy with Tm-170 seeds in this experimental model is more efficient than with I-125 seeds since Tm-170 emits both beta and gamma radiation and its gamma radiation range is higher than that of I-125
Keywords: Brachytherapy, Thulium-170 Seeds, Iodine-125 Seeds, Beta-Gamma Treatment.
INTRODUCTION
Interstitial brachytherapy is a method for radiation delivery to tumors that maximizes exposure to the tumor volume while minimizing toxicity to adjacent normal tissue (1-4). This technique exploits different principles of radiation physics; it delivers a controlled, concentrated, low dose rate to the tumor. Brachytherapy involves the stereotact deposition of permanent or removable radioactive implants of iodine-125 (28.4 keV), (5�8), iridium-192 (0.38 Mev), (9, 10), or palladium-103 (21 keV) (11, 12) directly into the tumor with continuous interstitial radiation, delivering cumulative doses of 30 to 120 Gy. (13,14) The benefit of brachytherapy is that the dose is delivered directly to the tumor, thereby reducing the dose to surrounding organs, unlike external beam radiotherapy, where radiation must traverse normal tissue to reach the tumor. Brachytherapy can be used intra-operatively in situations where surgery is not possible or not optimal or in situations where prior dose-limiting external radiotherapy has already been given. Combined approaches of surgery and brachytherapy can often improve the results of surgery alone in a variety of malignancies.
The radiobiology of LDR radiation is such that sub-lethal radiation damage in normal tissue is better repaired than in tumor tissue. Thus, the therapeutic window between normal and tumor tissue is further improved. (15).
We have developed a new brachytherapy seed based on thulium, Tm-170 which has several advantages over the ones in use. It emits both beta and gamma radiation therefore it is useful for short and long distances, its half life is much longer than that of Ir-192 therefore can be used for longer time before replaced.
Tm-170 seeds were made of 4.46 mg � 0.1 mg of thulium (0.2 � 0.6 � 4 mm; 9.32 g/cm3 density) inside titanium tubes of 0.8 mm outer diameter, 0.7 mm inner diameter, and 7 mm long
. Seeds were sealed by titanium plugs, which were inserted into the tubes using mechanical force. Each seed was individually placed inside a quartz ampoule and all ampoules were sent for neutron activation at the Soreq Nuclear Center (17).
The activity of the seeds was calculated using the equation 1.
A = N � σ � Φ � (1-e �λt0) (1)
N- Number of thulium atoms.
N = m (g) � Av (atoms/mole)/Aw (gr/mole) (2)
N = 1.59 � 1019 Atoms
σ- Cross section for activation, where the thermal neutron cross-section for Tm-169 captures a neutron and becomes Tm-170 is 105 b (17).
Φ- Neutron flux of 1 � 1013 n/cm2 s (17).
t0- Time of irradiation (23 hours or 82.8 thousand seconds)
λ- Decay constant
λ = ln2/T1/2 (3)
T1/2 = 128.6 days (18)
λ = 6.238 � 10-8 s-1
The calculated activity of the seeds was 2.54 mCi. This activity was chosen so that the photon dose from these seeds is about the same as that from the 0.5 mCi I-125 seeds calibrated by the supplier, this will be shown later using TLD dosimetry, to calibrate each seed and compare the gamma and X-ray doses from both kinds of seeds.
1.2. Tm-170 Emitted Photons
Tm-170 emits four major X-ray photons (7.4, 51.354, 52.389, and 59.4 keV) and one γ-ray (84.253 keV). The abundance of these photons as a function of their energy is given in Table 1. (18)
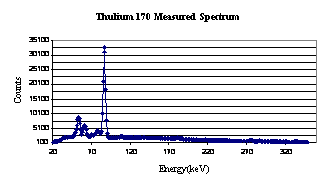
The photon spectrum of the Tm-170 seed (Figure 1) was measured with an H. P. Germanium (Z = 32) detector. Our results are similar to those reported by Crouthamel. (19)
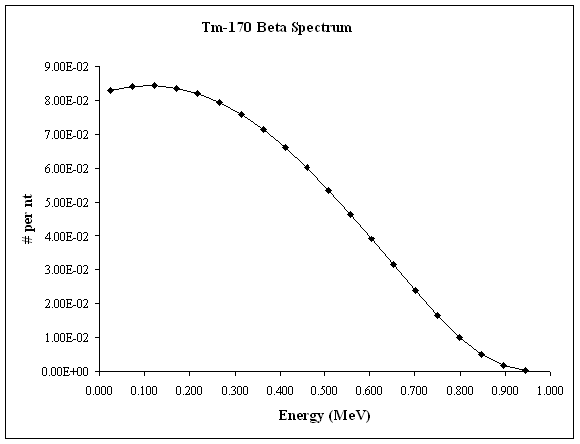
Tm-170 beta spectrum as described by Eckerman et al, (20) and Burrows (21) is shown in Figure 2. The beta emission from the Tm-170 source is summarized in Table 2; adding a large radiation dose to the 3.5 mm volume surrounding the seed.
2. Iodine 125 seeds
Iodine-125 seeds are popular LDR brachytherapy sources for prostate cancer therapy; I-125 seeds of nominal activity of 0.5 mCi are permanently implanted into the prostate, delivering cumulative doses of 30 to 120 Gy to the tumor.
Iodine-125 has a half-life of approximately 60 days. Iodine-125�s major spectrum is X-ray photons with energy of 27 and 31 keV. The photon emission of I-125 is shown in Table 3.
Iodine-125 seeds (Best Medical International, Inc.) with activity of 0.5mCi � 0.5 % as calibrated by the supplier are used.
Dosimetry of the seeds was carried out in cylindrical Perspex phantom made of two cylinders 10 cm diameter 9.5 cm height (one cylinder was used as a cover), with a perforation at the center where seeds could be placed. Six LiF (Mg, Ti) crystals 3.2 � 3.2 � 0.9 mm were placed in grooves at different distances and different angles around the source. (22)
Corrections were made for the energy dependency of the TLD sensitivity.
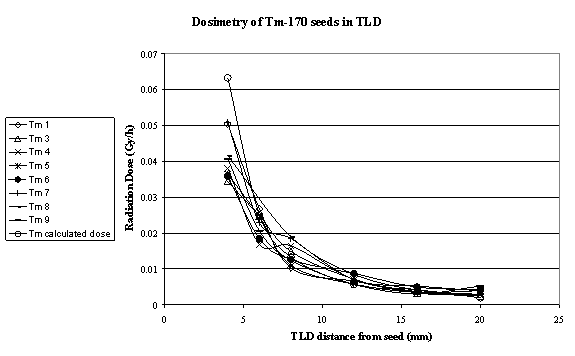
Dose from Tm-170 seeds was accumulated for 10 minutes. (Table 4 and Figure 3).
Beta particles were absorbed within the 3.5 mm radius surrounding the seed; therefore there was no contribution to the dose as measured using the TLD's method.
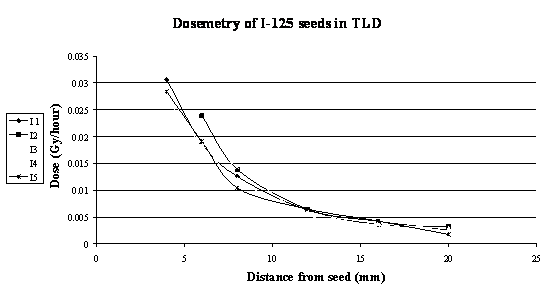
Dosimetry results of the I-125 seeds are shown in Figure 4 and Table 5.
Dosimetry of Tm-170 and I-125, shows a somewhat higher dose rate from Tm-170 seeds
4.1 The KHJJ murine mammary carcinoma
The Institutional Ethical Committee for Animal Research approved all animal studies.
The KHJJ radio-resistant murine mammary carcinoma (gift from Dr. Sara C. Rockwell, Yale University) was selected as the tumor model (23). The tumor was maintained by transplanting tumor fragments in Balb/c mice (Harlen Laboratories, Rehovot, Israel). Tumor fragments removed from mice may be also frozen for further use. Tumors reaching a volume of 400 mm3 were resected from a sacrificed mouse and gently minced in sterile saline. The tumor fragments were centrifuged and resuspended in 1 ml of 0.2 μm filtered freezing solution: Waymouth�s medium (Bet Hemek, Israel) supplemented with 15% FBS (Hyclone), 2% Pen/Strep solution (Bet Hemek,) and 15% glycerol (Sigma). One ml of tumor fragments suspension was transferred to a tightly closed ampoule; frozen at -20�C for 24 hours then transferred to liquid nitrogen for long term storage.
3.2 Implantation of KHJJ Tumors into BALB/C mice
Ten to twelve weeks old female BALB/C mice were used for implantation of KHJJ tumors. Each mouse was ear tagged and anesthetized with 80mg/kg Ketamine (FortDodge) and 8mg/kg Rompun (VMD). The right thigh was shaved and sterilized with 70% ETOH. A frozen ampoule containing the tumor fragments was defrosted and its content transferred in sterile conditions to a Petri dish. Using sharp sterile scissors a small (~ 1mm) cut was made in the thigh of the anesthetized mouse. A small tumor fragment was gently inserted under the skin with a sterile trochar. Antibacterial/fungal ointment (Synthomycine 5%) was used to cover the implanted area.
Mice were weighted three times a week to monitor their health. Growing tumors were palpable in 5 days and measurable by day 7. By day 25, their volume approached 400 mm3. Mice showing signs of distress or bearing 400 mm3 tumors were sacrificed with CO2. Tumor growth was monitored every other day, using a digital caliper (24, 25). Tumor volume was determined by measurement of length (l), width (w), and height (h); corrections for the ellipsoidal shape of tumor were made using the formula: (23)
Volume = п/6 � l � w � h mm3
The KHJJ tumor grows exponentially with time. Tumors reaching 7�8 mm length were chosen for implantation with radioactive seeds. This tumor size was chosen because the Tm-170 seeds have a length of 7�8 mm (the radioactive Tm-170 in the seed is only 4 mm in length). Characteristic volumes of tumors of such length are 30�100 mm3, depending on their dimensions.
4.1. Brachytherapy Using Thulium-170 Seeds Compared to Iodine-125 Commercial Seeds
A comparison between the therapeutic benefits of I-125 and the new source�Tm-170� is the subject of this work.
Tm-170 and Iodine-125 seeds were implanted into mice bearing KHJJ tumors. The tumor dimensions at the time of implantation were typical 65 mm3 average.
Both Iodine-125 and Thulium-170 seeds were kept inside the tumors until the tumors either disappeared, at which time seeds were surgically removed, or the tumors had grown to a volume of ~ 400 mm3 when mice were sacrificed and seeds removed. Using a computer-generated random number table, tumor-bearing mice were randomized into 4 groups of 20 mice:
A. Control group 1, no treatment.
B. Control group 2, implantation of dummy seeds.
C. Experimental group 1, implantation of I-125 seeds.
D. Experimental group 2, implantation of Tm-170 seeds.
Four of the I-125 seeds fell off the tumors; therefore only results of 16 mice are presented).
Cure, delay in tumor growth, or undisturbed growth was determined according to tumor volume at the end-point.
4.2 Seed implantation procedure
An anesthetized mouse was fixed on a platform behind lead glass; a trochar (similar to those used for seed implantation in patients), was introduced into the tumor .The trochar was loaded with a sterile seed and pushed into the center of the tumor. The seed implantation procedure is shown in Figure 5.
Single mice were kept protected from irradiation by other mice with 3 mm thick lead sheets between their cages. Tumors were measured with a caliper behind a 3 cm thick lead glass.
Results
Brachytherapy Using Thulium-170 Seeds Compared to Iodine-125
1. Control 1 � no treatment
Tumors in mice that did not receive any treatment grew exponentially with time. Tumors reached a volume of 400 mm3 within 15�25 days from implantation (Figure 6).
2. Control 2 �Dummy seeds implanted KHJJ tumors
Dummy seeds are empty titanium capsules with the same dimensions as the Tm-170 seeds; they were activated together of the Tm-170 seeds at the Soreq Nuclear Center. There was no measurable radiation from these seeds.
No effect was expected from these seeds on the tumors and, as expected, the tumors grew exponentially (Figure 7). Most of these tumors reached a volume of 400 mm3 within 15�25 days. A small delay in growth of some tumors was observed and is attributed to the cuts made in the tumor for the implantation procedure, which caused a leakage of a small amount of necrotic liquid from the center of the tumor.
3. Iodine-125 seeds implanted tumors
The tumor growth is shown in Figures 8, and 9, and 10, were 25% of the cases are considered as full success (cure), 25% of partial success (delay in tumor growth) and 50% of failure.
Fully cured mice (within 25-30 days) were kept for observation and did not develop recurrent tumors.
Mice in which tumors grew slower, reached a volume of 400 mm3 more than 30 days after implantation.
4. Thulium-170 Seeds implanted tumors
Tumor growth is shown in Figures 11, 12, and 13. As can be seen, implantation of Tm-170 seeds resulted in 60% success, 20 % of partial success and 20% of failure.
Discussion
60% of tumors regressed following implantation of Tm-170 seeds into KHJJ tumors, while I-125 seeds of the same photon dose resulted only in 25% cure. Tm-170 as a successful brachytherapy source is most likely due to the fact that Tm-170 emits beta rays of energy up to 960 keV (average energy 315 keV), ignoring self absorption of the beta particles in the source, a very high dose rate is produced by the beta particles (about 270 Gy/hour), which leads to the improved results of Tm-170 over I-125 seeds.
Moreover, Tm-170 emits photons of energy higher than those of the I-125; these photons have enough energy to reach distant cells and have the ability to treat large tumors.
Photon range is defined as 1/�, where � is the energy attenuation coefficient. For photons with energies of 51, 59, and 84 keV emitted from a Tm-170 source, the range in water is 23.7, 31.3, and 38.5 cm, respectively.
The Thulium-170 radioactive decay spectrum includes 5.75% photons of energy above 50 keV (photons of energy below 7�9 keV emitted in small quantity); the rest of the dose is due to beta rays of high energy and well-defined range. Iodine-125, on the other hand, emits more than 1 photon for each nuclear decay for a total output of ~140%, the main energy of these photons is 27 keV; these photons have a range of about 6.4 cm in water.
Despite the fact that I-125 emits photons with intensity 24 times higher than that of Tm-170, Tm-170 proved to be a much better isotope.
The photon dose distributions as a function of distance from the source starting at 4 mm are shown in Figs. 3 and 7. The dose 6 mm from the source is about 2.2 cGy/h for Tm-170 seeds and about 2 cGy/h for the I-125 seeds.
As seen in the figure the radiation dose of I-125 falls off faster than that from Tm-170. This is due to the higher energy of the Tm-170 photon. Thus the dose due to photons, at shorter distance, is higher for I-125. At longer distance the photon dose from Tm-170 is higher.
Study accuracy limitation
There are two major parameters in the present study which set the limits of its accuracy; these are the number of mice and seeds doses.
For practical reasons the number of mice in each group was limited to 20. This number imposes an accuracy limit of � 22 %. The statistical accuracy of the results obtained with 20 mice in a group is generally acceptable (26). The uncertainty in the dose is due to uncertainty in the seeds activity. Although the Tm-170 seeds were prepared exactly the same way, the amount of Tm-169 in each seed varied with a maximum error of 1-2 %. The possible error might be due to small variation in the neutron flux at which the seeds were irradiated. A small deviation from the activation spot in the reactor may cause deviations in the activity. This can be seen in figure 3. At distances smaller than 8 mm from the source, the range of the dose rate is within a factor of 1.5 (at 4 mm it is between 0.034 Gy/h to 0.05 Gy/h).
The I-125 seeds activity was measured by the supplier and was guarantied to be within � 5%.
Another possible error may be introduced by the uncertainty of using the caliper to measure the tumor dimensions due to the irregularity of tumor shape. To reduce variability, the same person made all the measurements. We estimate that the measurements are accurate within � 0.3 mm i.e. an error of the order of 5 %.
Acknowledgments
This research was supported by the Israeli Ministry of Science, Culture and Sport as a part of the program supporting Ph.D. students for Israeli Arab citizens.
The authors would like to thank
Dr. Ela Wiener and Mrs. Irit Levinger for their expert technical support.
References
1. G. P. Murphy, W. Lawrence and R.E. Lenhard, American Cancer Society Textbook of CLINICAL ONCOLOGY, 2nd ed. American Cancer Society, Atlanta, GA ,1995.
2. L. L. Anderson, R. Nath, K.A. Weaver, D. Nori, T.L.Phillips, Y. H. Son, S. T. Chiu Tsao, A. S. Meigooni, J. A. Meli and V. Smith (Interstitial Collaborative Working Group), Interstitial Brachytherapy, physical, biological and clinical considerations. Raven Press, New York, 1990.
3. J. F. Williamson, Physics of Brachytherapy. In Principles and Practice of Radiation Oncology (Perez CA, Brady LW, Eds) 3rd ed, pp. 405-467. PA: Lippincott-Raven Press, Philadelphia, 1997.
4. R.W. Kline. Comment on Dosimetry of interstitial brachytherapy sources: Recommendations of the AAPM Radiation Therapy Committee Task Group No. 43. Med. Phys. 23, 1579 (1996).
5. T. P. Loftus. Exposure standardization of I-125 seeds used for brachytherapy. J Res Natl Bur Stand 89, 295-303 (1984).
6. B. S. Hilaris, J. G. Holt and J. St. Germain. The Use of Iodine-125 for interstitial Implants, DHEW Publication (FDA) 76-8022. Rockville, Maryland: U.S. Department of Health, Education and Welfare, 1975.
7. Y. Yu, L. L. Anderson, Z. Li, D. E. Mellenberg, R. Nath, M. C. Schell, F. M. Waterman, A. Wu, and J. C. Blasko, Permanent prostate seed implant brachytherapy: Report of the American Association of Physicists in Medicine Task Group No. 64, Med. Phys. 26, 2054-2076 (1999).
8. K. Wallner, J. Roy and L. Harrison, Tumor control and morbidity following transperineal iodine 125 implantation for stage T1/T2 prostatic carcinoma. J Clin Oncol. 14, 449�453 (1996).
9. G. P. Glasgow and L. T. Dillman, Specific- ray constant and exposure rate constant for Ir-192. Med. Phys. 6, 49-52 (1979).
10. S. Deger, D. Boehmer, J. Roigas, T. Schink, K. Wernecke, T. Wiegel, W. Hinkelbein, V. Budach and S. Loening. High dose rate (HDR) brachytherapy with conformal radiation therapy for localized prostate cancer. European Urology 47(4), 441-448 (2005).
11. J. Sharkey, A. Cantor, Z. Solc, W. Huff, S. D. Chovnick, R. J. Behar, R. Perez, J. Otheguy and R. Rabinowitz, Pd-103 brachytherapy versus radical prostatectomy in patients with clinically localized prostate cancer: a 12-year experience from a single group practice. Brachytherapy 4, 34�44 (2005).
12. A. S. Meigooni, S. Sabnis and R. Nath, Dosimetry of Pd-103 brachytherapy sources for permanent implant. Endocurietherapy Hypertherm Oncol. 6, 107-117 (1990).
13. R. Nath, L. L. Anderson, G. Luxton, K. A. Weaver, J. F. Williamson and A. S. Meigooni, Dosimetry of interstitial brachytherapy sources: Recommendations of the AAPM Radiation Therapy Committee Task Group No. 43. Med. Phys. 22, 209-234 (1995).
14. M. J. Rivard, B. M. Coursey, L. A. DeWerd, W. F. Hanson, M. Saiful Huq, G. S. Ibbott, M. G. Mitch, R. Nath and J. F. Williamson, Update of AAPM Task Group No. 43 Report: A revised AAPM protocol for brachytherapy dose calculations.
15. E. J. Hall, Radiobiology for the Radiologist, 5th Ed. Lippincott Williams and Wilkins, New York, 2000.
16. A. Hwaree, I. Orion and G. Shani, Development of New Brachytherapy Seeds based on Tm-170. 5th International Conference on Isotopes. Brussels, Belgium, Book of Abstracts, 25-29 April (2005).
17. Israel Atomic Energy Commission, Yavne 81800, Israel.
18. http://www.nndc.bnl.gov/.
19. C. E. Crouthamel, Applied Gamma-Ray Spectrometry, 2nd ed. Pergamon Press, Oxford, New York, 1970.
20. K. F. Eckerman, R. J. Westfall, J. C. Ryman and M. Cristy, Availability of Nuclear Decay Data in Electronic Form, Including Beta Spectra not Previously Published. Health Phys. 67(4), 338-345 (1994).
21. T. W. Burrows. The Program RADLST. Brookhaven National Laboratory, Report BNL-NCS-52142, 1988.
22. A. Ayoub, Development of new radioactive seeds Tm-170 for brachytherapy combined with Auger electron emission. Ph.D. Thesis, Ben Gurion University, Beer Sheva Israel, 2007.
23. S. C. Rockwell, R. F. Kallman and L. F. Fajardo, Characteristics of a Serially Transplanted Mouse Mammary Tumor and its Tissue-Culture-Adapted Derivative. Journal of the National Cancer Institute 49, 735-749 (1972).
24. D. Duguay, F. Mercier, J. Stagg, D. Martineau, J. Bramson, M. Servant, R. T. Lin, J. Galipeau and J. Hiscott, In Vivo Interferon Regulatory Factor 3 Tumor Suppressor Activity in B Melanoma Tumors. Cancer Research 62, 5148-5152 (2002).
25. S. W. Nam, T. Clair, C. K. Campo, H. Y. Lee, L. A. Liotta and M. L. Stracke, Autotaxin (ATX), a potent tumor motogen, augments invasive and metastatic potential of ras-transformed cells. Oncogene, 19, 241-247 (2000).
26. J. C. Verhoeff, L. JA. Stalpers, A. W. Coumou, K. Koedooder, C. Lavini, C. JF. Van Noorden, J. Haveman, W. P. Vandertop and W. R. Van Furth, Experimental iodine-125 seed irradiation of intracerebral brain tumors in nude mice. Radiation Oncology, 2, 38 (2007).
List of Figures
|
1 |
Thulium-170 Measured Spectrum |
|
2 |
Tm-170 beta spectrum |
|
3 |
Radiation dose from Tm-170 seed measured in TLD crystals |
|
4 |
Radiation dose from I-125 seed measured in TLD crystals |
|
5 |
Seed implantation procedure |
|
6 |
Control tumor growth as a function of time |
|
7 |
Tumor growth as a function of time, implantation of dummy seeds |
|
8 |
Tumor volumes as a function of time, cured mice- I-125 |
|
9 |
Tumor volumes as a function of time, tumors progression - I-125 |
|
10 |
Tumor volumes as a function of time, tumors not affected - I-125 |
|
11 |
Tumor volumes as a function of time, cured mice � Tm-170 |
|
12 |
Tumor volumes as a function of time, tumors progression � Tm-170 |
|
13 |
Tumor volumes as a function of time, tumors not affected � Tm-170 |
List of Tables
|
1 |
Thulium-170 Photons |
|
2 |
Tm-170 beta emission products |
|
5 |
I-125 photon emission products |
|
4 |
Dosimetry of Tm-170 in TLD Radiation detectors |
|
5 |
Dosimetry of I-125 in TLD Radiation detectors |

![]()
![]()









|
Photon Energy (keV) |
Abundance |
|
7.42 |
0.040326 |
|
51.354 |
0.012748 |
|
52.389 |
0.022483 |
|
59.4 |
0.009301 |
|
84.253 |
0.032552 |
|
|
Maximum |
Average |
|
Fraction |
Energy (MeV) |
Energy (Mev) |
|
0.24 |
0.883 |
0.290 |
|
0.76 |
0.967 |
0.323 |
|
Relative Fraction |
Energy (MeV ( |
|
0.064 |
0.035 |
|
0.154 |
0.0037 |
|
0.254 |
0.031 |
|
0.392 |
0.027 |
|
0.731 |
0.027 |
|
|
Radiation Dose (mrem/hour) � Tm-170 seeds |
|||||||
|
TLD distance from source (mm) |
Seed 1 |
Seed 3 |
Seed 4 |
Seed 5 |
Seed 6 |
Seed 7 |
Seed 8 |
Seed 9 |
|
4 |
5034 |
3438 |
3804 |
3642 |
3588 |
5070 |
4152 |
4068 |
|
6 |
2676 |
2478 |
1686 |
2454 |
1842 |
2286 |
- |
2058 |
|
8 |
1032 |
1488 |
1650 |
1098 |
1266 |
1848 |
1896 |
1248 |
|
12 |
666 |
714 |
708 |
582 |
876 |
708 |
852 |
576 |
|
16 |
372 |
336 |
366 |
354 |
498 |
528 |
414 |
312 |
|
20 |
294 |
264 |
282 |
396 |
420 |
396 |
288 |
528 |
|
|
Radiation Dose (mrem/hour) � I-125 seeds |
||||
|
TLD distance from source (mm) |
Seed 1 |
Seed 2 |
Seed 3 |
Seed 4 |
Seed 5 |
|
4 |
3056 |
- |
2684 |
2884 |
2840 |
|
6 |
1876 |
2384 |
1884 |
1820 |
1908 |
|
8 |
1256 |
1392 |
1200 |
1436 |
1044 |
|
12 |
628 |
644 |
604 |
536 |
648 |
|
16 |
424 |
360 |
388 |
356 |
428 |
|
20 |
260 |
316 |
280 |
232 |
176 |